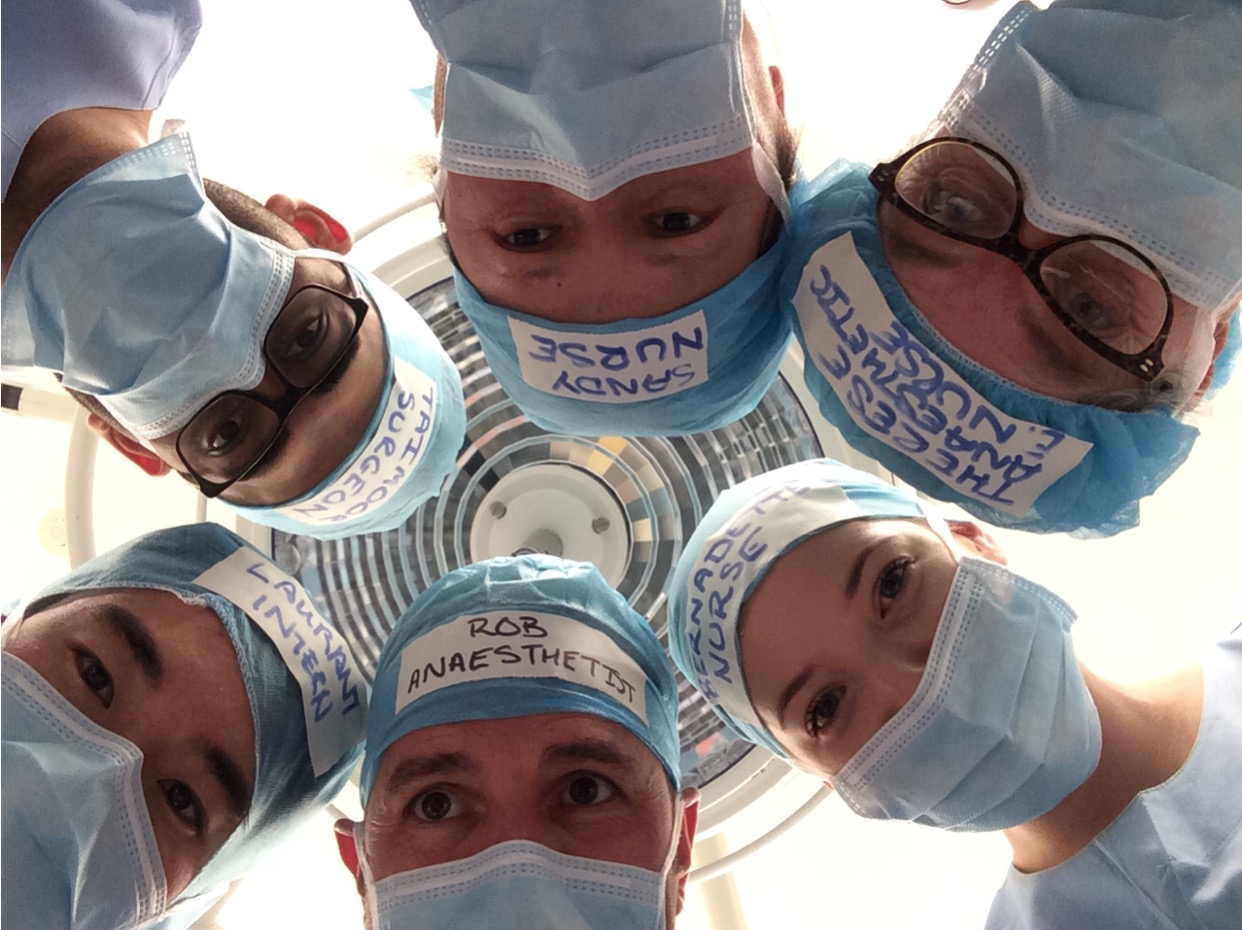
The patient declined rapidly, the arrest call went out, staff rushed into the operating room. Some helped obtain intravenous access, others drew up adrenaline, and the arrest trolley was brought in. As the patient’s cardiac output disappeared the anaesthetist asked for someone to commence cardiac compressions then turned to put the patient on 100% oxygen. On turning back he noticed compressions hadn’t started. The anaesthetist made eye contact with a nurse and asked her to start compressions – she looked behind thinking he meant someone else. The anaesthetist realised, despite having worked in the same hospital as the nurse for years, he didn’t know her name. Moments later another staff member stepped in.
Perhaps these vital few moments may have made the difference to the patient’s outcome.
Medical error has been reported as the third greatest cause of death – we can overcome this.
Knowing someone’s name allows clearer, more direct, communication – it’s a non-technical skill. Non-technical skills refer to general cognitive and social skills that allow one to, among other things, monitor a situation, make decisions, take a leadership role, communicate and co-ordinate actions within a team, in order to achieve high levels of safety and efficiency. There is growing awareness that non-technical skills are essential for competent practice and improved patient outcomes.
The World Health Organisation Team Time Out process involves staff introducing themselves providing their name and role. This step is in response to poor communication being recognised as contributory to numerous adverse events. Unfortunately, given lack of transparency with error reporting, operating theatre staff aren’t aware of the significance of this issue (see here). While this box is invariably ticked, the actual process is trivialised and rarely takes place – this is the gap that exists between work as perceived and work as performed (see here).

Knowing one another’s names instils camaraderie and improves social interaction in a workplace.
Sometimes names are written on a white board in theatre – these whiteboards obviously don’t move with the staff member. Many theatre staff work in several different operating rooms and even in different hospitals. Remembering everyone’s name in the constantly shifting workforce is an almost impossible task. Names are forgotten and staff frequently pass the stage where asking someone’s name becomes too socially awkward.
From the patient’s perspective when everyone appears the same it is extremely difficult and unsettling to discern who is who.
Policies exist in many institutions indicating that staff clearly display their name and role above waist height. These policies don’t translate well into operating theatres – badges and lanyards are viewed as an infection risk and become covered under sterile, lead or other gowns. For the most part staff in operating theatres have no visible means of identification.
A simple solution to this problem is for staff to have their names and roles written onto their surgical hats. Essentially this places no extra work onto the front line – names which would have otherwise been written on a white board, are written on the staff member instead.
So why aren’t we already doing this?
Perhaps for fear of looking ridiculous. However, as this great TED talk reveals, all movements must start somewhere:
Perhaps administrators view a label on one’s head as a message of imperfection. If we forget people’s names what else might we forget? Unfortunately this is how hospitals are invariably designed – on the premise that as doctors and nurses we shouldn’t make mistakes. However we’re just as human as everyone else, just as likely to make mistakes, yet these mistakes frequently lead to catastrophic outcomes.
We need to nurture a culture which allows us to redesign our healthcare institutions. We need to develop systems which reduce mistakes and minimise them from causing harm when they inevitably occur. For this to happen, we need to let everyone know we’re human.
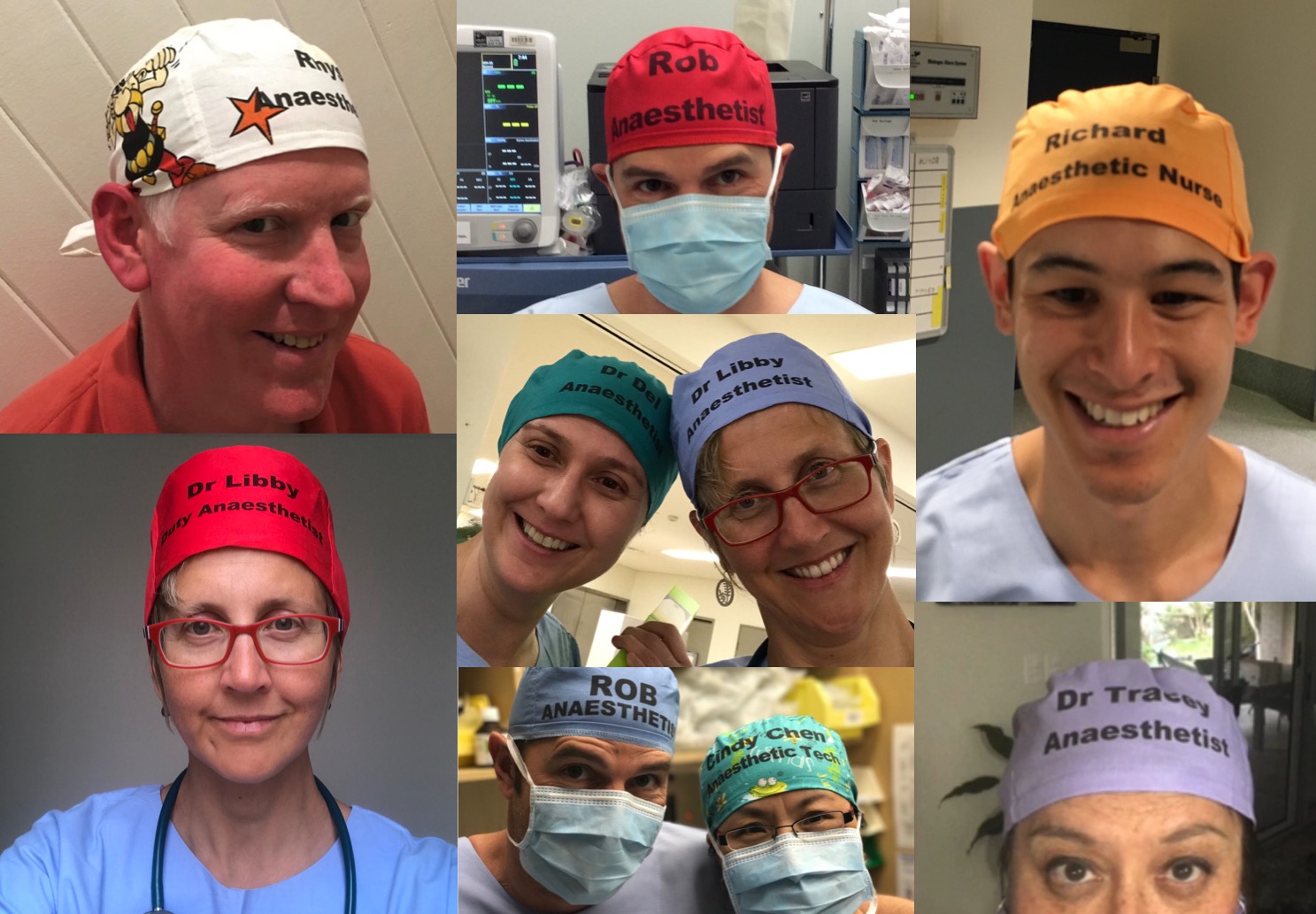
Willing to let others know you’re human to improve patient safety? #knowyourhuman
You can order theatre hats with your name & role through Hunter Scrubs via this link: click here.
Hunter Scrubs ship internationally.
Please note we have no financial interest with Hunter Scrubs or anything else discussed on the PatientSafe Network.
There is no clear evidence to support use of disposable surgical hats over cotton hats from an infection perspective. This single centre trial has studied infection rates extensively: see here. We acknowledge that despite this many institutions do not allow cloth hats – we will keep you updated on a more aesthetic sticker system we are trialling.
Dr Rhys Thomas – Anaesthesia Quality & Safety Fellow brilliantly explains the importance of theatre hats imprinted with names and roles in this video: ‘What’s in a name?’
If patient safety is to improve we need frameworks which generate a safety culture (see here).
Thank you for your support.


14 Comments